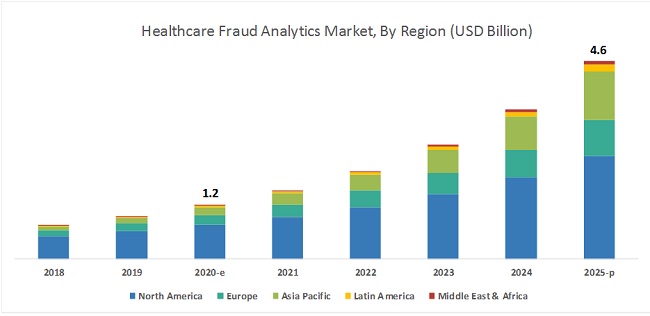
Healthcare fraud analytics market growth can be attributed to the large number of fraudulent activities in healthcare; the increasing number of patients seeking health insurance; high returns on investment; and rising pharmacy claim-related frauds.
What the Healthcare Fraud Analytics Market Looks Like?
The healthcare fraud analytics market is projected to reach USD 4.6 billion by 2025 from USD 1.2 billion in 2020, at a CAGR of 29.8%. North America market to witness the highest growth during the forecast period.
Download PDF Brochure @ https://www.marketsandmarkets.com/pdfdownloadNew.asp?id=221837663
Based on the solution type, the descriptive analytics segment accounted for the largest share of the market in 2019. Descriptive analytics forms the base for the effective application of predictive or prescriptive analytics. Hence, these analytics use the basics of descriptive analytics and integrate them with additional sources of data in order to produce meaningful insights.
On the basis of application, the healthcare fraud detection market is segmented into insurance claims review, pharmacy billing misuse, payment integrity, and other applications. In 2019, the insurance claims review segment dominated the healthcare fraud analytics market. The increasing number of patients seeking health insurance, the rising number of fraudulent claims, and the growing adoption of the prepayment review model are expected to drive the growth of this segment in the coming years.
What Drives the Healthcare Fraud Analytics Market?
The growth of the global market for Healthcare Fraud Analytics is primarily influenced by the following factors:
Large Number of Fraudulent Activities in Healthcare
Increasing Number of Patients Seeking Health Insurance
Prepayment Review Model
High Returns on Investment
Rise in Pharmacy Claims-Related Fraud
However, the dearth of skilled personnel is likely to restrain the growth of healthcare fraud detection market.
Please provide your specific interest in this report so as to help you better , Request a Sample Pages @ https://www.marketsandmarkets.com/requestsampleNew.asp?id=221837663
Geographical growth scenario of Healthcare Fraud Detection Market
Geographically, the global healthcare fraud detection market is segmented into North America, Europe, the Asia Pacific, Latin America, and the Middle East and Africa. North America accounted for the largest share of the market in 2019. The high share of the North American market is attributed to the large number of people having health insurance, growing healthcare fraud, favorable government anti-fraud initiatives, the pressure to reduce healthcare costs, technological advancements, and greater product and service availability in this region. Moreover, a majority of leading players in the healthcare fraud detection market have their headquarters in North America.
Leading healthcare fraud detection market players and strategies adopted
IBM Corporation (US), Optum (US), SAS Institute (US), Change Healthcare (US), EXL Service Holdings (US), Cotiviti (US), Wipro Limited (India), Conduent (US), HCL (India), Canadian Global Information Technology Group (Canada), DXC Technology Company (US), Northrop Grumman Corporation (US), LexisNexis Group (US), and Pondera Solutions (US).
For more details, Speak to Analyst @ https://www.marketsandmarkets.com/speaktoanalystNew.asp?id=221837663